nauliza kwa doctor yeyote ugonjwa uitwao Staphylococas ni upi kuna mgonjwa kapimwa na pia dawa za antibiotics kama tetracline,cipro,amoxciln,pennicilin hazijamtibu baada ya kuweka kwenye culture,hebu nielezee na madhara yake na dawa ipi atumie kwani ni mdada anaumia tumbo la uzazi.
Navigation
More options
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
dawa kuwa immune kwa binadamu.
- Thread starter Eyoma
- Start date
Herbalist Dr MziziMkavu
JF-Expert Member
- Feb 3, 2009
- 42,314
- 33,108
What is Staphylococcus?
Staphylococcus is a group of bacteria that can cause a number of diseases as a result of infection of various tissues of the body. Staphylococcus is more familiarly known as Staph (pronounced "staff"). Staph-related illness can range from mild and requiring no treatment to severe and potentially fatal.
The name Staphylococcus comes from the Greek staphyle, meaning a bunch of grapes, and kokkos, meaning berry, and that is what Staph bacteria look like under the microscope, like a bunch of grapes or little round berries. (In technical terms, these are gram-positive, facultative anaerobic, usually unencapsulated cocci.)
Over 30 different types of Staphylococci can infect humans, but most infections are caused byStaphylococcus aureus. Staphylococci can be found normally in the nose and on the skin (and less commonly in other locations) of around 25%-30% of healthy adults and in 25% of hospital workers. In the majority of cases, the bacteria do not cause disease. However, damage to the skin or other injury may allow the bacteria to overcome the natural protective mechanisms of the body, leading to infection.
Who is at risk for Staph infections?
Anyone can develop a Staph infection, although certain groups of people are at greater risk, including newborn infants, breastfeeding women, and people with chronic conditions such as diabetes, cancer, vascular disease, and lung disease. Injecting drug users, those
with skin injuries or disorders, intravenous catheters, surgical incisions, and those with a weakened immune system due either to disease or a result of immune suppressing medications all have an increased risk of developing Staph infections.
Staph infections are contagious until the infection has resolved. Direct contact with an infected sore or wound, or with personal-care items such as razors, bandages, etc., are common routes of transmission. Casual contact such as kissing or hugging does not pose a great risk for transmission if there is no direct contact with the infected area.
What are the symptoms and signs of a Staph infection?
Staphylococcal disease of the skin usually results in a localized collection of pus, known as an abscess, boil, or furuncle, depending upon the exact type of lesion that is present. The affected area may be red, swollen, and painful. Drainage or pus is common. When Staph is in the blood (bacteremia orsepsis), it can cause high fevers, chills, and low blood pressure.
What types of diseases are caused by Staph?
Skin infections (see above) are the most common type of disease produced by Staphylococcus. Staph infections of the skin can progress to impetigo (a crusting of the skin) orcellulitis (inflammation of the deeper layers of skin and connective tissue under the skin, leading to swelling and redness of the area). In rare situations, a serious complication known as scalded skin syndrome (see below) can develop. Inbreastfeeding women, Staph can result in mastitis (inflammation of the breast) or in abscess of the breast. Staphylococcal breast abscesses can release bacteria into the mother's milk.
When the bacteria enter the bloodstream and spread to other organs, a number of serious infections can occur. Spread of the organisms to the bloodstream is known as bacteremia or sepsis. Staphylococcal pneumoniapredominantly affects people with
underlying lung disease and can lead to abscess formation within the lungs. Infection of the heart valves (endocarditis) can lead to heart failure. Spread of Staphylococci to the bones can result in severe inflammation of the bones known asosteomyelitis.
When Staph bacteria are present in the blood, a condition known as staphylococcal sepsis (widespread infection of the bloodstream) or staphylococcal bacteremia exists. Staphylococcal sepsis is a leading cause of shock and circulatory collapse,
leading to death, in people with severe burns over large areas of the body. When untreated, Staph aureussepsis carries a mortality (death) rate of over 80%. Although not common,Staph aureus has been reported as a cause of chorioamnionitis and neonatal sepsis in pregnancy, but group B streptococci are the most common bacterial cause of this life-threatening condition for the fetus.
Staphylococcal infections are contagious and can be transmitted from person to person. Since pus from infected wounds may contain the bacteria, proper hygiene and hand washing is required when caring for Staph-infected wounds.
Staphylococcal food poisoning is an illness of the bowels that causesnausea, vomiting, diarrhea, and dehydration. It is caused by eating foods contaminated with toxins produced by Staphylococcus aureus rather than a true infection with the bacteria.
Symptoms usually develop within one to six hours after eating contaminated food. The illness usually lasts for one to three days and resolves on its own. Patients with this illness are not contagious since toxins are not transmitted from one person to another.
Toxic shock syndrome is an illness caused by toxins secreted by Staph aureus bacteria growing under conditions in which there is little or no oxygen. Toxic shock syndrome is characterized by the sudden onset of highfever, vomiting, diarrhea, and
muscle aches, followed by low blood pressure(hypotension), which can lead to shock and death. There may be a rashresembling sunburn, with peeling of skin. Toxic shock syndrome was originally described and still occurs especially in menstruating women using tampons.
Staphylococcus is a group of bacteria that can cause a number of diseases as a result of infection of various tissues of the body. Staphylococcus is more familiarly known as Staph (pronounced "staff"). Staph-related illness can range from mild and requiring no treatment to severe and potentially fatal.
The name Staphylococcus comes from the Greek staphyle, meaning a bunch of grapes, and kokkos, meaning berry, and that is what Staph bacteria look like under the microscope, like a bunch of grapes or little round berries. (In technical terms, these are gram-positive, facultative anaerobic, usually unencapsulated cocci.)
Over 30 different types of Staphylococci can infect humans, but most infections are caused byStaphylococcus aureus. Staphylococci can be found normally in the nose and on the skin (and less commonly in other locations) of around 25%-30% of healthy adults and in 25% of hospital workers. In the majority of cases, the bacteria do not cause disease. However, damage to the skin or other injury may allow the bacteria to overcome the natural protective mechanisms of the body, leading to infection.
Who is at risk for Staph infections?
Anyone can develop a Staph infection, although certain groups of people are at greater risk, including newborn infants, breastfeeding women, and people with chronic conditions such as diabetes, cancer, vascular disease, and lung disease. Injecting drug users, those
with skin injuries or disorders, intravenous catheters, surgical incisions, and those with a weakened immune system due either to disease or a result of immune suppressing medications all have an increased risk of developing Staph infections.
Staph infections are contagious until the infection has resolved. Direct contact with an infected sore or wound, or with personal-care items such as razors, bandages, etc., are common routes of transmission. Casual contact such as kissing or hugging does not pose a great risk for transmission if there is no direct contact with the infected area.
What are the symptoms and signs of a Staph infection?
Staphylococcal disease of the skin usually results in a localized collection of pus, known as an abscess, boil, or furuncle, depending upon the exact type of lesion that is present. The affected area may be red, swollen, and painful. Drainage or pus is common. When Staph is in the blood (bacteremia orsepsis), it can cause high fevers, chills, and low blood pressure.
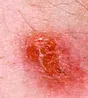
|
| What does a Staph infection look like? |
What types of diseases are caused by Staph?
Skin infections (see above) are the most common type of disease produced by Staphylococcus. Staph infections of the skin can progress to impetigo (a crusting of the skin) orcellulitis (inflammation of the deeper layers of skin and connective tissue under the skin, leading to swelling and redness of the area). In rare situations, a serious complication known as scalded skin syndrome (see below) can develop. Inbreastfeeding women, Staph can result in mastitis (inflammation of the breast) or in abscess of the breast. Staphylococcal breast abscesses can release bacteria into the mother's milk.
When the bacteria enter the bloodstream and spread to other organs, a number of serious infections can occur. Spread of the organisms to the bloodstream is known as bacteremia or sepsis. Staphylococcal pneumoniapredominantly affects people with
underlying lung disease and can lead to abscess formation within the lungs. Infection of the heart valves (endocarditis) can lead to heart failure. Spread of Staphylococci to the bones can result in severe inflammation of the bones known asosteomyelitis.
When Staph bacteria are present in the blood, a condition known as staphylococcal sepsis (widespread infection of the bloodstream) or staphylococcal bacteremia exists. Staphylococcal sepsis is a leading cause of shock and circulatory collapse,
leading to death, in people with severe burns over large areas of the body. When untreated, Staph aureussepsis carries a mortality (death) rate of over 80%. Although not common,Staph aureus has been reported as a cause of chorioamnionitis and neonatal sepsis in pregnancy, but group B streptococci are the most common bacterial cause of this life-threatening condition for the fetus.
Staphylococcal infections are contagious and can be transmitted from person to person. Since pus from infected wounds may contain the bacteria, proper hygiene and hand washing is required when caring for Staph-infected wounds.
Staphylococcal food poisoning is an illness of the bowels that causesnausea, vomiting, diarrhea, and dehydration. It is caused by eating foods contaminated with toxins produced by Staphylococcus aureus rather than a true infection with the bacteria.
Symptoms usually develop within one to six hours after eating contaminated food. The illness usually lasts for one to three days and resolves on its own. Patients with this illness are not contagious since toxins are not transmitted from one person to another.
Toxic shock syndrome is an illness caused by toxins secreted by Staph aureus bacteria growing under conditions in which there is little or no oxygen. Toxic shock syndrome is characterized by the sudden onset of highfever, vomiting, diarrhea, and
muscle aches, followed by low blood pressure(hypotension), which can lead to shock and death. There may be a rashresembling sunburn, with peeling of skin. Toxic shock syndrome was originally described and still occurs especially in menstruating women using tampons.
Herbalist Dr MziziMkavu
JF-Expert Member
- Feb 3, 2009
- 42,314
- 33,108
How are Staph infections diagnosed?
In cases of minor skin infections, staphylococcal infections are commonly diagnosed by their appearance without the need for laboratory testing. More serious staphylococcal infections such as infection of the bloodstream, pneumonia, and endocarditis require culturing of samples of blood or infected body fluids. The laboratory establishes the diagnosis and performs special tests to determine which antibiotics are effective against the bacteria.
What is the treatment for Staph infections?
Minor skin infections are usually treated with an antibiotic ointment such as a nonprescription triple-antibiotic mixture. In some cases, oral antibiotics may be given for skin infections. Additionally, if abscesses are present, they are surgically drained. More serious and life-threatening infections are treated with intravenous antibiotics. The choice of antibiotic depends on the susceptibility of the particular staphylococcal strain as determined by culture results in the laboratory. Some Staph strains, such as MRSA (see next section), are resistant to many antibiotics.
What is antibiotic-resistant Staph aureus?
Methicillin-resistant Staphylococcus aureus, known as MRSA, is a type ofStaphylococcus aureus that is resistant to the antibiotic methicillin and other drugs in the same class, including penicillin, amoxicillin, and oxacillin. MRSA is one example
of a so-called "superbug," an informal term used to describe a strain of bacteria that has become resistant to the antibiotics usually used to treat it. MRSA first appeared in patients in hospitals and other health facilities, especially among the elderly, the very sick, and those with an open wound (such as a bedsore) or catheter in the body. In these settings, MRSA is referred to as health care-associated MRSA (HA-MRSA).
MRSA has since been found to cause illness in the community outside of hospitals and other health facilities and is known as community-associated MRSA (CA-MRSA) in this setting. MRSA in the community is associated with recent antibiotic use, sharing contaminated items, having active skin diseases or injuries, poor hygiene, and living in crowded settings. The U.S.
Centers for Disease Control and Prevention (CDC) estimates that about 12% of MRSA infections are now community-associated, but this percentage can vary by community and patient population.
MRSA infections are usually mild superficial infections of the skin that can be treated successfully with proper skin care and antibiotics. MRSA, however, can be difficult to treat and can progress to life-threatening blood or bone infections because there are fewer effective antibiotics available for treatment.
The transmission of MRSA is largely from people with active MRSA skin infections. MRSA is almost always spread by direct physical contact and not through the air. Spread may also occur through indirect contact by touching objects (such as towels,
sheets, wound dressings, clothes, workout areas, sports equipment) contaminated by the infected skin of a person with MRSA. Just as S. aureus can be carried on the skin or in the nose without causing any disease, MRSA can be carried in this way also.
In contrast to the relatively high (25%-30%) percentage of adults who are colonized by Staph aureus in the nose (these people have Staph bacteria present that do not cause illness), only about 2% of healthy people carry MRSA in the nose. There are no
symptoms associated with carrying Staph in general or MRSA in the nose.
A drug known as mupirocin (Bactroban) has been shown to be effective in some cases for treating and eliminating MRSA from the nose of healthy carriers, but decolonization (treating of carriers to remove the bacteria) is usually not recommended unless
there has been an outbreak of MRSA or evidence that an individual or group of people may be the source of the outbreak.
More recently, strains of Staph aureus have been identified that are resistant to the antibiotic vancomycin (Vancocin), which is normally effective in treating Staph infections. These bacteria are referred to as vancomycin-intermediate-resistance S. aureus (VISA) and vancomycin-resistant Staph aureus (VRSA).
What are complications of Staph infections?
Scalded skin syndrome is a potentially serious side effect of infection with Staph bacteria that produce a specific protein which loosens the "cement" holding the various layers of the skin together. This allows blister formation and sloughing of the top layer of skin. If it occurs over large body regions, it can be deadly, similar to a large surface area of the body having been
burned. It is necessary to treat scalded skin syndrome with intravenous antibiotics and to protect the skin from allowing dehydration to occur if large areas peel off. The disease occurs predominantly in children but can occur in anyone. It is known formally as staphylococcal scalded skin syndrome.
Staph Infection (Staphylococcus Aureus) Symptoms, Causes, Photos, Treatment - MedicineNet
In cases of minor skin infections, staphylococcal infections are commonly diagnosed by their appearance without the need for laboratory testing. More serious staphylococcal infections such as infection of the bloodstream, pneumonia, and endocarditis require culturing of samples of blood or infected body fluids. The laboratory establishes the diagnosis and performs special tests to determine which antibiotics are effective against the bacteria.
What is the treatment for Staph infections?
Minor skin infections are usually treated with an antibiotic ointment such as a nonprescription triple-antibiotic mixture. In some cases, oral antibiotics may be given for skin infections. Additionally, if abscesses are present, they are surgically drained. More serious and life-threatening infections are treated with intravenous antibiotics. The choice of antibiotic depends on the susceptibility of the particular staphylococcal strain as determined by culture results in the laboratory. Some Staph strains, such as MRSA (see next section), are resistant to many antibiotics.
What is antibiotic-resistant Staph aureus?
Methicillin-resistant Staphylococcus aureus, known as MRSA, is a type ofStaphylococcus aureus that is resistant to the antibiotic methicillin and other drugs in the same class, including penicillin, amoxicillin, and oxacillin. MRSA is one example
of a so-called "superbug," an informal term used to describe a strain of bacteria that has become resistant to the antibiotics usually used to treat it. MRSA first appeared in patients in hospitals and other health facilities, especially among the elderly, the very sick, and those with an open wound (such as a bedsore) or catheter in the body. In these settings, MRSA is referred to as health care-associated MRSA (HA-MRSA).
MRSA has since been found to cause illness in the community outside of hospitals and other health facilities and is known as community-associated MRSA (CA-MRSA) in this setting. MRSA in the community is associated with recent antibiotic use, sharing contaminated items, having active skin diseases or injuries, poor hygiene, and living in crowded settings. The U.S.
Centers for Disease Control and Prevention (CDC) estimates that about 12% of MRSA infections are now community-associated, but this percentage can vary by community and patient population.
MRSA infections are usually mild superficial infections of the skin that can be treated successfully with proper skin care and antibiotics. MRSA, however, can be difficult to treat and can progress to life-threatening blood or bone infections because there are fewer effective antibiotics available for treatment.
The transmission of MRSA is largely from people with active MRSA skin infections. MRSA is almost always spread by direct physical contact and not through the air. Spread may also occur through indirect contact by touching objects (such as towels,
sheets, wound dressings, clothes, workout areas, sports equipment) contaminated by the infected skin of a person with MRSA. Just as S. aureus can be carried on the skin or in the nose without causing any disease, MRSA can be carried in this way also.
In contrast to the relatively high (25%-30%) percentage of adults who are colonized by Staph aureus in the nose (these people have Staph bacteria present that do not cause illness), only about 2% of healthy people carry MRSA in the nose. There are no
symptoms associated with carrying Staph in general or MRSA in the nose.
A drug known as mupirocin (Bactroban) has been shown to be effective in some cases for treating and eliminating MRSA from the nose of healthy carriers, but decolonization (treating of carriers to remove the bacteria) is usually not recommended unless
there has been an outbreak of MRSA or evidence that an individual or group of people may be the source of the outbreak.
More recently, strains of Staph aureus have been identified that are resistant to the antibiotic vancomycin (Vancocin), which is normally effective in treating Staph infections. These bacteria are referred to as vancomycin-intermediate-resistance S. aureus (VISA) and vancomycin-resistant Staph aureus (VRSA).
What are complications of Staph infections?
Scalded skin syndrome is a potentially serious side effect of infection with Staph bacteria that produce a specific protein which loosens the "cement" holding the various layers of the skin together. This allows blister formation and sloughing of the top layer of skin. If it occurs over large body regions, it can be deadly, similar to a large surface area of the body having been
burned. It is necessary to treat scalded skin syndrome with intravenous antibiotics and to protect the skin from allowing dehydration to occur if large areas peel off. The disease occurs predominantly in children but can occur in anyone. It is known formally as staphylococcal scalded skin syndrome.
Staph Infection (Staphylococcus Aureus) Symptoms, Causes, Photos, Treatment - MedicineNet
gfsonwin
JF-Expert Member
- Apr 12, 2012
- 18,274
- 20,673
MziziMkavu umesema vizuri sana, juu ya hawa staphylococci ila nafikiri kwakuwa watanzania wengi huwa hawana ujuzi wa hizi scientific names basi ni bora muda mwingine tuwe tunatumia common names. Mathalani hali ya kuwa na painful skin lension, red, hot and which gives out puss mwanabiolojia ataelewa ila mwingine hataweza kuunganisha vizuri so use its common name kwamba n majipu au sijui jipu likiwa moja. Hayo ni kwa mujibu wangu tu and am sorry kama mwalimu nitakuwa nimeingilia kazi ya daktari
Last edited by a moderator:
Herbalist Dr MziziMkavu
JF-Expert Member
- Feb 3, 2009
- 42,314
- 33,108
@gfsonwin thank you Teacher, your always welcome.MziziMkavu umesema vizuri sana, juu ya hawa staphylococci ila nafikiri kwakuwa watanzania wengi huwa hawana ujuzi wa hizi scientific names basi ni bora muda mwingine tuwe tunatumia common names. Mathalani hali ya kuwa na painful skin lension, red, hot and which gives out puss mwanabiolojia ataelewa ila mwingine hataweza kuunganisha vizuri so use its common name kwamba n majipu au sijui jipu likiwa moja. Hayo ni kwa mujibu wangu tu and am sorry kama mwalimu nitakuwa nimeingilia kazi ya daktari
gfsonwin
JF-Expert Member
- Apr 12, 2012
- 18,274
- 20,673
@gfsonwin thank you Teacher, your always welcome.
Nashukuru sana wewe daktari kukubali ushauri wa huyu mwalimu.
Herbalist Dr MziziMkavu
JF-Expert Member
- Feb 3, 2009
- 42,314
- 33,108
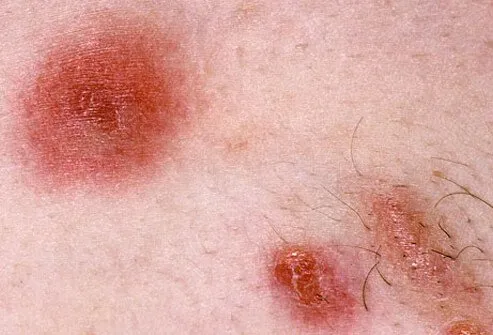
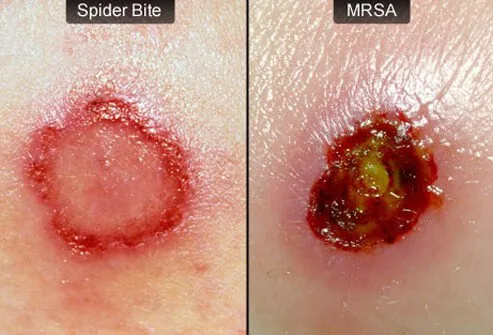
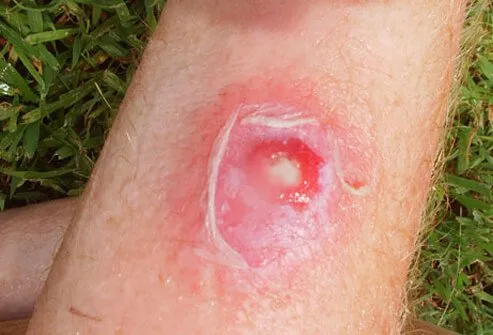
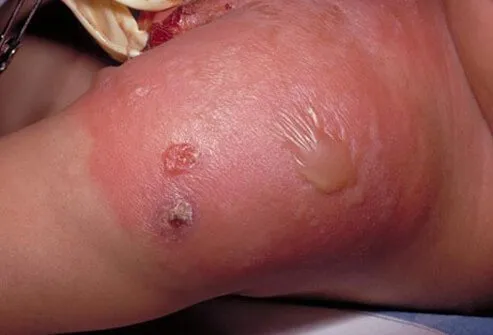
What Types of Diseases Are Caused by Staph?
Skin infections are the most common type of disease produced by Staphylococcus. Staph infections of the skin can progress to impetigo (a crusting of the skin) or cellulitis (inflammation of the connective tissue under the skin, leading to swelling and redness of the area). In breastfeeding women, Staph can result in mastitis (inflammation of the breast) or in abscess of the breast. Staphylococcal breast abscesses can release bacteria into the mother's milk. When the bacteria enter the bloodstream and spread to other organs (known as bacteremia or sepsis), a number of serious infections can occur such as staphylococcal pneumonia, infection of the heart valves (endocarditis, which can lead to heart failure), and osteomyelitis (severe inflammation of the bones). Staphylococcal sepsis is a leading cause of shock and circulatory collapse, leading to death, in people with severe burns over large areas of the body. When untreated, Staph aureus sepsis carries a mortality (death) rate of over 80%.
Last edited by a moderator:
gfsonwin
JF-Expert Member
- Apr 12, 2012
- 18,274
- 20,673
Duh! umenikumbusha nilipokuwa nasoma somo liitwalo medical microbiology ambapo..........lol haya makitu hadi kinyaa jamani yaani tuliyapanda na kuyastain sitak kukumbuka hadi yamenifanya nimekuwa mwoga wa vitu vingi sana but atleast ile basic knowlege ya vijidudu ninayo na hata kukachungulia kwenye microscope naweza. but for medical practitioners you real need risk allowance
Similar Discussions
-
SoC02 Matumizi holela ya dawa za binadamu yanaathari kubwa Sana kwa mtumiaji
- Started by Adqcos
- Replies: 0
-
Tuzifahamu familia 13 za Illuminati zinazoiendesha dunia na maisha ya binadamu katika nyanja zote
- Started by Jackwillpower
- Replies: 96
-
Waziri Ummy, Usipotoshwe maamuzi yako kuhusu ADDO na wafamasia mtawaumiza Watanzania
- Started by Prof Koboko
- Replies: 350
-
-